Summary
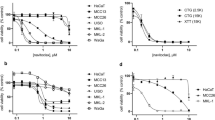
Pharmacological treatments for psoriasis are generally based on antiproliferative, anti-inflammatory, or differentiation-modifying activity, or a combination of two or more of these actions. Potentially new drugs for treatment of psoriasis, which act on proliferation, can be identified by screening large compound libraries in a cell proliferation model that allows for characterization of drug effects on in vitro growth of normal human keratinocytes. High-throughput programs based on biological testing of diverse collections of compounds can rapidly identify leads for potential drug candidates in the treatment of psoriasis. In this study, we describe nonradioactive measurement of keratinocyte proliferation in the exponential growth phase in a 96-well format, using a sensitive deoxyribonucleic acid-binding dye to analyze drugs that are pharmacologically active in growth inhibition. Release of lactate dehydrogenase was used to exclude cytotoxic effects. We examined a number of compounds in a test range of 10−7 to 10−5 M, including known antipsoriatic drugs, and experimental drugs that are potentially useful in the treatment of psoriasis. We found strong concentration-dependent growth inhibition by dithranol, an antipsoriatic compound that is presumed to target the epidermal compartment. Methotrexate, cyclosporin A, and all-trans retinoic acid did not significantly affect proliferation at therapeutically relevant concentrations. The p38 mitogen-activated protein kinase inhibitor, SB220025, and curcumin, a natural phytochemical, inhibited keratinocyte proliferation at 10−5 M. We conclude that this assay, in combination with the previously developed assays for psoriatic differentiation, provides a useful tool for identification of antipsoriatic drugs.
Similar content being viewed by others
References
Bharti, A. C.; Donato, N.; Singh, S.; Aggarwal, B. B. Curcumin (diferuloylmethane) downregulates the constitutive activation of nuclear factor {kappa}B and I{kappa}B{alpha} kinase in human multiple myeloma cells leading to suppression of proliferation and induction of apoptosis. Blood 101:1053–1062;2003.
Blaheta, R. A.; Kronenberger, B.; Woitaschek, D., et al. Development of an ultrasensitive in vitro assay to monitor growth of primary cell cultures with reduced mitotic activity. J. Immunol. Methods 211:159–169; 1998.
Chaudhari, U.; Romano, P.; Mulcahy, L. D.; Dooley, L. T.; Baker, D. G.; Gottlieb, A. B. Efficacy and safety of infliximab monotherapy for plaque-type psoriasis: a randomised trial. Lancet 357:1842–1847;2001.
Chen, Y. R.; Tan, T. H. Inhibition of the c-jun N-terminal kinase (JNK) signaling pathway by curcumin. Oncogene 17:173–178;1998.
Cheng, A. L.; Hsu, C. H.; Lin, J. K., et al. Phase I clinical trial of curcumin, a chemopreventive agent, in patients with high-risk or pre-malignant lesions. Anticancer Res. 21:2895–2900;2001.
Dengler, W. A.; Schulte, J.; Berger, D. P.; Mertelsmann, R.; Fiebig, H. H. Development of a propidium iodide fluorescence assay for proliferation and cytotoxicity assays. Anticancer Drugs 6:522–532; 1995.
Dykes, P. J.; Brunt, J.; Marks, R. The effect of cyclosporin on human epidermal keratinocytes in vitro. Br. J. Dermatol. 122:137–180, 1990.
Fisher, G. J.; Duell, E. A.; Nickoloff, B. J.; Annesley, T. M.; Kowalke, J. K.; Ellis, C. N.; Voorhees, J. J. Levels of cyclosporin in epidermis of treated psoriasis patients differentially inhibit growth of keratinocytes cultured in serum free versus serum containing media. J. Invest. Dermatol. 91:142–146; 1988.
Gottlieb, A. B.; Khandke, L.; Krane, J. F.; Staiano-Coico, L.; Ashinoff, R.; Krueger, J. G. Anthralin decreases keratinocyte TGF-alpha expression and EGF-receptor binding in vitro. J. Invest. Dermatol. 98:680–685; 1992.
Ieiri, I.; Nakayama, J.; Murakami, H.; Hori, Y.; Higuchi, S. Evaluation of the therapeutic range of whole blood cyclosporin concentration in the treatment of psoriasis. Int. J. Clin. Pharmacol. Ther. 34:106–111; 1996.
Jeffes, E. W., III; Lee, G. C.; Said, S., et al. Elevated numbers of proliferating mononuclear cells in the peripheral blood of psoriatic patients correlate with disease severity. J. Invest. Dermatol. 105:733–738; 1995a.
Jeffes, E. W., III; McCullough, J. L.; Pittelkow, M. R., et al. Methotrexate therapy of psoriasis: differential sensitivity of proliferating lymphoid and epithelial cells to the cytotoxic and growth-inhibitory effects of methotrexate. J. Invest. Dermatol. 104:183–188; 1995b.
Katayama, H.; Kawada, A. Exacerbation of psoriasis induced by indomethacin. J. Dermatol. 8:323–327; 1981.
Konger, R. L.; Malaviya, R.; Pentland, A. P. Growth regulation of primary human keratinocytes by prostaglandin E receptor EP2 and EP3 subtypes. Biochim. Biophys. Acta 1401:221–234; 1998.
Lee, J. C.; Laydon, J. T.; McDonnell P. C., et al. A protein kinase involved in the regulation of inflammatory cytokine biosynthesis. Nature 372:739–746; 1994.
Mukhopadhyay, A.; Bueso-Ramos, C.; Chatterjee, D.; Pantazis, P.; Aggarwal, B. B. Curcumin downregulates cell survival mechanisms in human prostate cancer cell lines. Oncogene 20:7597–7609; 2001.
Nakamura, K.; Yasunaga, Y.; Segawa, T.; Ko, D.; Moul, J. W.; Srivastava, S.; Rhim, J. S. Curcumin down-regulates AR gene expression and activation in prostate cancer cell lines. Int. J. Oncol. 21:825–830; 2002.
Nickoloff, B. J.; Fisher, G. J.; Mitra, R. S.; Voorhees, J. J. Additive and synergistic antiproliferative effects of cyclosporin A and gamma interferon on cultured human keratinocytes. Am. J. Pathol. 131:12–18; 1988.
Pentland, A. P.; Needleman, P. Modulation of keratinocyte proliferation in vitro by endogenous prostaglandin synthesis. J. Clin. Invest. 77:246–251; 1986.
Pfundt, R.; Wingens, M.; Bergers, M.; Zweers, M.; Frenken, M.; Schalkwijk, J. TNF-alpha and serum induce SKALP/elafin gene expression in human keratinocytes by a p38 MAP kinase-dependent pathway. Arch. Dermatol. Res. 292:180–187; 2000.
Pol, A.; Bergers, M.; van Ruissen, F.; Pfundt, R.; Schalkwijk, J. A simple technique for high-throughput screening of drugs that modulate normal and psoriasis-like differentiation in cultured human keratinocytes. Skin Pharmacol. Appl. Skin Physiol. 15:252–261; 2002.
Schwartz, P. M.; Kugelman, L. C.; Coifman, Y.; Hough, L. M.; Milstone, L. M. Human keratinocytes catabolize thymidine. J. Invest. Dermatol. 90:8–12; 1988.
Sharpe, G. R.; Fisher, C. Time-dependent inhibition of growth of human keratinocytes and fibroblasts by cyclosporin A: effect on keratinocytes at therapeutic blood levels. Br. J. Dermatol. 123:207–213; 1990.
Sorensen, S.; Solvsten, H.; Politi, Y.; Kragballe, K. Effects of vitamin D3 on keratinocyte proliferation and differentiation in vitro: modulation by ligands for retinoic acid and retinoid X receptors. Skin Pharmacol. 10:144–152; 1997.
van Ruissen, F.; de Jongh, G. J.; Zeeuwen, P. L.; van Erp, P. E.; Madsen, P.; Schalkwijk, J. Induction of normal and psoriatic phenotypes in submerged keratinocyte cultures. J. Cell. Physiol. 168:442–452; 1996.
Varani, J.; Nickoloff, B. J.; Dixit, V. M.; Mitra, R. S.; Voorhees, J. J. All-trans retinoic acid stimulates growth of adult human keratinocytes cultured in growth factor-deficient medium, inhibits production of thrombos-pondin and fibronectin, and reduces adhesion. J. Invest. Dermatol. 93:449–454; 1989.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pol, A., Bergers, M. & Schalkwijk, J. Comparison of antiproliferative effects of experimental and established antipsoriatic drugs on human kerationocytes, using a simple 96-well-plate assay. In Vitro Cell.Dev.Biol.-Animal 39, 36–42 (2003). https://doi.org/10.1290/1543-706X(2003)039<0036:COAEOE>2.0.CO;2
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1290/1543-706X(2003)039<0036:COAEOE>2.0.CO;2